Premier Prosthetics Center in East Tennessee
At Choice Orthotics & Prosthetics, we take an integrated approach to prosthetic care. To us, we believe that we are not just replacing your limb, we are giving you back the mobility, freedom and quality of life you deserve.
We believe that no two people are created equal. That explains why we customize our prosthetic solutions based on individual patient’s needs. Our Board-Certified Prosthetist experts makes and fits a wide range of lower and upper extremity prostheses customized to best meet or surpass your goals and lifestyle.
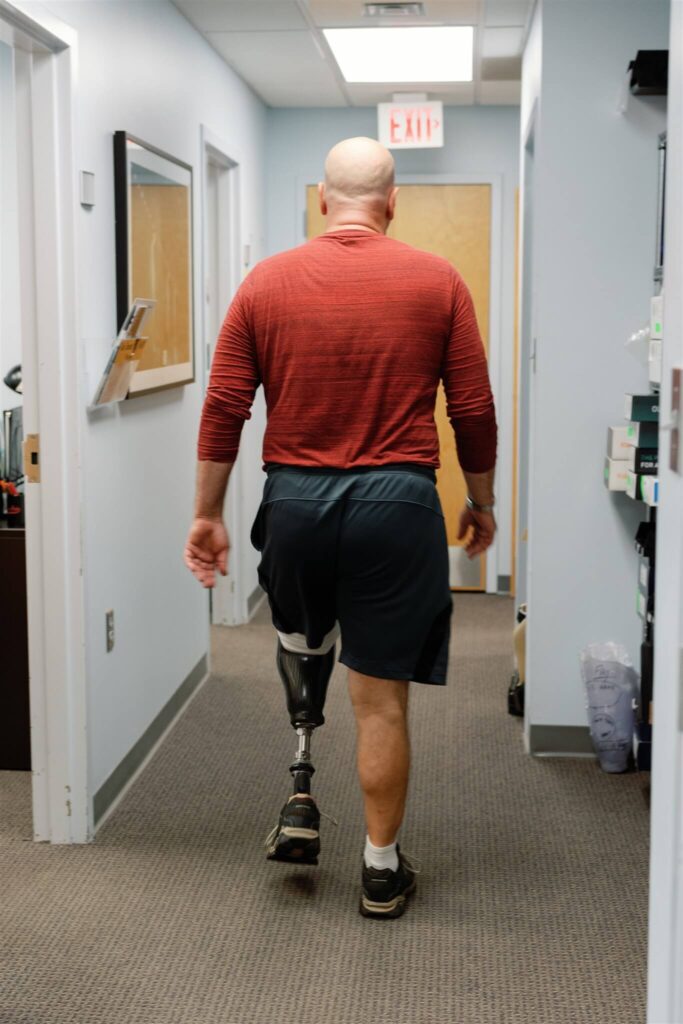

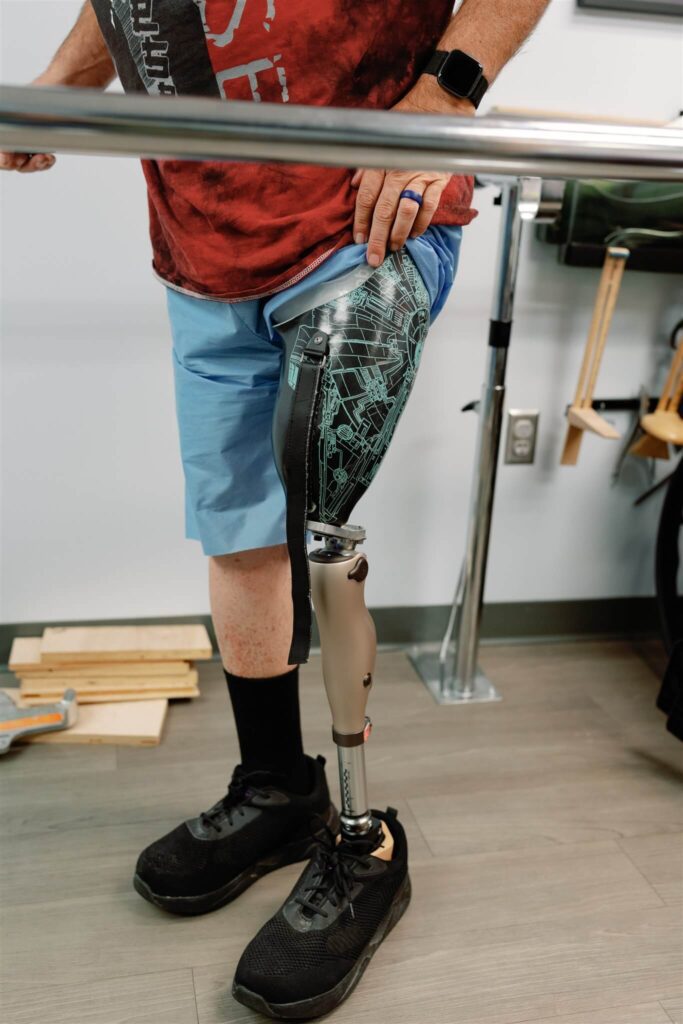
At Choice Orthotics & Prosthetics, we have experienced clinicians who will use the latest prosthetic technology to help patients attain their vitality goals. We use a proven approach to prosthetic care that makes this transition easy on you and your family. The partnership between our clinicians and Prosthetist Experts ensures that you regain your life without any hassle.
As a premier Prosthetics & Orthotics provider in East Tennessee, we pride ourselves on our ability to offer a wide range of cutting-edge prosthetic products crafted in our onsite lab. We equip patients to maximize opportunities in life through instant access to the leading limb technology and prosthetic solutions.
With our fabrication lab located in Murfreesboro, our experts will design, fabricate and maintain your prostheses locally. We never send your prostheses to an outside team because we don’t want to lose oversight and control of its craftmanship and quality. Our lab develops state-of-the-art options for both lower and upper body extremities.
We are committed to offering you the latest in prosthetic and orthotic technologies, superior care and specialized training. Our process provides superior function and fit, even for those patients who have been dissatisfied with comfort and performance offered by prosthetic components from other service providers.
At Choice Orthotics & Prosthetics, we offer a wide selection of innovative and the most advanced prosthetic solutions in East Tennessee to match your lifestyle and goals. Contact your nearest Choice Orthotics & Prosthetics location to schedule a free consultation, and experience our comprehensive care for yourself.

Initial Evaluation
We provide no obligation initial assessment to evaluate your current situation and identify how our services can benefit you most.

Fabricate
After assessment, our fabrication team will craft your custom prosthesis to allow for successful mobility.

Fix and Adjust
After delivering your prosthesis, our clinicians will continue to help ensure your device is working seamlessly.

Follow Up With You
Our team will schedule ongoing appointments to follow up on whether our unique prosthetic solution has improved your quality of life.



